Diagnosing Osteo Arthritis Through Imaging
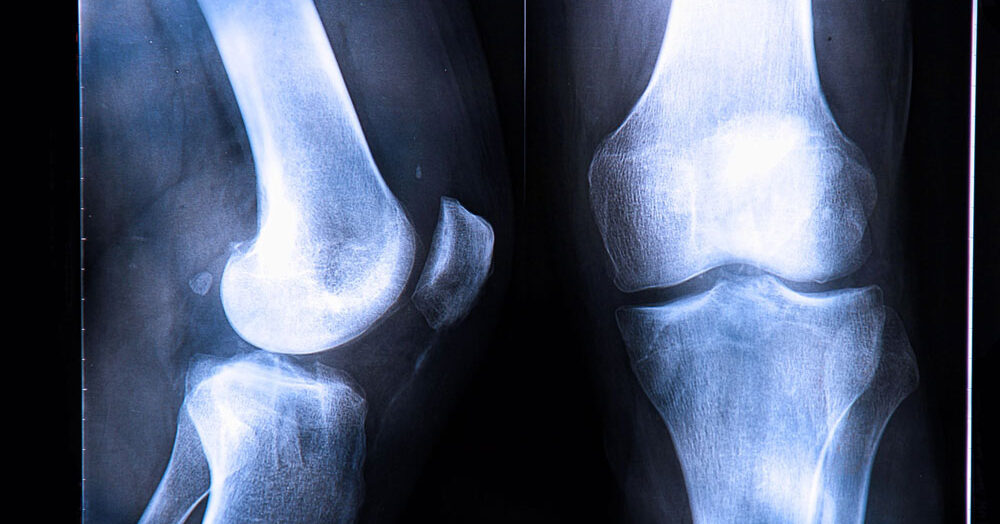
Imaging is useful for diagnosing and monitoring the progression of osteo arthritis. It can show medical professionals more accurate results than traditional radiography.
Osteo arthritis is a term that refers to a set of overlapping joint problems, which can affect a single joint or many joints of varying sizes1.
If not treated well, these osteo arthritic joints can cause severe pain and prevent you from doing the activities you like. As part of a holistic treatment plan, a knee brace can help reduce osteo arthritis pain.
In this article, we’ll discuss the role of imaging in diagnosing and managing knee osteo arthritis.
What Exactly Is the Role of Imaging in Diagnosing Osteo Arthritis (OA)?
Imaging is a powerful tool for diagnosing and managing osteo arthritis. It helps medical professionals to confirm their diagnosis of osteo arthritis and assist those who are experiencing a fast development of their symptoms.
Research shows that improved imaging performance indicators such as CT scans, MRI, and ultrasounds have better accuracy and responsiveness to conventional radiography2.
How Does Osteo Arthritis Occur?
Degeneration of articular cartilage eventually leads to osteo arthritis. This often occurs on its own as a natural part of the aging process. It can also occur as a secondary condition resulting from a related injury. These can include a traumatic injury, injury caused by repetitive stress, or injury sustained on the job.
Articular cartilage degradation is a slow process that takes some time to develop in natural aging osteo arthritis3. As a result, there are several stages of osteoarthritis that classify its severity based on the level of cartilage degradation. The radiographic imaging findings depend on the stage of osteo arthritis that a person has.
The stages of osteo arthritis are:
- Mild
- Moderate
- Severe
- Localized
- Diffuse
Types of Imaging Technologies for OA
1. Conventional/Traditional Radiographs
One of the imaging types used to diagnose osteo arthritis is a conventional radiograph, also known as a routine X-ray examination.
On conventional radiographs (X-rays), osteo arthritis has different features than other joint illnesses, such as rheumatoid arthritis. This is true for the knee joint and any other joints afflicted by the condition.
For example, a quality digital X-ray of a knee joint with patellofemoral osteoarthritis will show that the cartilage has worn away, leaving a decreased space between kneecap (patella) and thigh bone (femur). If you’re unfamiliar with the patellofemoral knee joint, here’s a useful resource to learn more.
In severe osteo arthritis, the cartilage is almost all gone and the bone starts to rub against bone. This can lead to cavities or cysts developing in the bone, which can also be detected by X-ray equipment.
Furthermore, a process called sclerosis can occur, where more bone forms in the spaces where cartilage used to be. As a result, the joint surfaces may become uneven, and osteophytes, also known as bone spurs, may develop.
In addition to traditional X-ray views, your physician may use advanced X-ray views in order to find early cartilage wear. This helps your doctor save time and make the traditional X-ray examination more sensitive.
2. Specialized/Advanced Diagnostic Imaging Exams of Osteo Arthritis
Osteo arthritis symptoms can manifest before it’s possible to detect the joint damage using conventional X-ray imaging. As a result, radiologists often use more sensitive imaging techniques, such as MRI, CT, and ultrasound. These are preferable for identifying the early stages of osteo arthritis.
Let’s take a closer look at these advanced imaging technologies:
CT Scan
Computed tomography (CT) exams are useful for showing osteophytes (bone spurs/spikes) and how they damage the soft tissues near them. CT scans can also be helpful in guiding diagnostic and therapeutic operations.
MRI
Magnetic resonance imaging (MRI) is a very sensitive imaging technique, so it can detect even the smallest changes in bone and soft tissues. An MRI can detect reactive bone edema – a build up of fluid in the bone marrow that causes swelling, soft tissue inflammation, and deteriorated cartilage/bone fragments stuck in the joint. Your physician can also identify early signs of cartilage deterioration with a procedure that uses specific MRI pulse patterns.
When early signs of cartilage wear are detected, therapy can help prevent or postpone the course of the condition. As a result, this may prevent or delay the requirement for surgical intervention4.
Ultrasound
Ultrasound evaluates the ligaments and tendons that surround the joints. Therefore, it is highly effective at detecting rips or strains caused by osteo arthritis. Also, ultrasound is an effective method for diagnosing synovial cysts, which are sometimes present in joints with osteoarthritis.
How to Manage OA
Your physician will utilize the information from your imaging tests to choose the best therapy for you. Treatment options for knee osteo arthritis include both non-surgical therapies and invasive surgical procedures.
Nonsurgical therapies include:
- Physical therapy
- Adjustments to physical activity
- Oral medicines
- Intra-articular steroid injections
- Knee bracing
Often a combination of non-surgical therapies is best for managing osteo arthritis. For example, a combination of knee bracing, injections, and an exercise program may help to decrease pain and improve mobility more than one therapy alone.
If you’re considering a knee brace, note that not all osteo arthritis knee braces function in the same way. Most braces use straps to shift your weight onto the healthy side of your knee, relieving pain in only one damaged compartment. However, a new bracing technology uses springs to lift weight off of the joint, providing pain relief across your entire knee. Physicians are moving towards spring technology, recognizing that it is the only bracing technology that can manage osteo arthritis as it progresses and spreads throughout the knee. Learn more about spring braces here.
If surgery is needed, your physician may recommend a partial or total knee replacement. They may also recommend an osteotomy, where a wedge of bone near the affected joint is removed.
How Does Imaging Help With OA Management?
Not only do radiographic technologies can assist with diagnosing knee osteo arthritis, they can also direct your physician in administering therapies for the condition.
For example, a physician may choose to use injections of anesthetics or long effecting steroids, which can be helpful in reducing the pain caused by the condition5. Imaging guidance helps them to observe that the needle tip is adequately put into the joint region during injection operations. CT, ultrasonography, or MRI can provide this sort of direct vision.
Arthrography is also possible due to these advanced imaging technologies. An arthrogram is an injection administered to a joint using fluoroscopy or CT guidance. First, the physician injects a small amount of contrast material into the joint so that they can see the needle more clearly and ensure it is in the right spot. Using ultrasonography, the radiologist is able to see the needle while it is inside the joint, in addition to the surrounding muscles and blood vessels. In this instance, the use of imaging can greatly improve the accuracy of the injection.
If you’re experiencing knee joint pain, here are some resources for information and solutions:
Pain on the Front of Your Knee Joint? Learn Why
Knee Pain on the Inside of Your Joint? Causes and Solutions
Knee Pain When Bending or Squatting? Learn Why
The Best Patellofemoral Knee Brace
References
1. https://pubmed.ncbi.nlm.nih.gov/27734845/
2. https://academic.oup.com/rheumatology/article/57/suppl_4/iv51/4812624
3. https://emedicine.medscape.com/article/392096-overview
4. https://pubmed.ncbi.nlm.nih.gov/24792944/
5. https://www.sciencedirect.com/science/article/pii/S1063458414011145